Measles
While vaccination has reduced the number of global deaths considerably, with a decrease of 73% from 2000 to 2018, between 150,000 and 200,000 people still die from this disease each year, predominantly children under five living in Sub-Saharan Africa. Furthermore, WHO recorded a 79% increase in global cases over the first two months of 2022 versus the same period in 2021. It appears that the upswing that started in 2016 is continuing, or even worsening, which reinforces the importance of continuing the fight against this infectious disease.
Measles is an infectious disease that mainly affects children. It is highly contagious, with one person estimated to contaminate between 15 and 20 others. Its symptoms are high fever, cough, nasopharyngitis, and then a rash. The initial symptoms are easily confused with those of other pathologies, and those who are infected are contagious before the characteristic rash appears and for up to five days afterwards, thus facilitating disease propagation.
Measles: A disease with no specific treatment
There is no specific treatment for the disease; only the symptoms are treated. Severe complications occur in approx. 30% of cases, mainly in children under five who are malnourished or have an immune disorder such as advanced HIV. The most severe complication is often pneumonia. In contexts where infant mortality is higher than 100 per 1,000 infants, the case fatality ratio of measles can exceed 5% (1). Furthermore, the virus destroys certain immune system cells in the first days of infection, making the infected person susceptible to other opportunistic infections.
Vaccine coverage still largely insufficient
An effective vaccine to prevent the disease has been available since the 1960s. Thanks to its introduction, the impact of measles and its associated mortality have been reduced. However, to eradicate the disease, 95% of the population must be immunised. Vaccine coverage is far from reaching this target in many countries.
Two doses of the vaccine are needed to guarantee increased immunity. A first injection is administered to infants between 9 and 11 months. In many countries, the second dose is only rarely administered. A 2021 publication (2) showed improved coverage with the first dose of the vaccine in 15 African countries (Benin, Burkina Faso, Cape Verde, Côte d’Ivoire, Gambia, Ghana, Guinea, Guinea-Bissau, Liberia, Mali, Niger, Nigeria, Senegal, Sierra Leone and Togo): from 45% in 2001 to 66% in 2019. However, only seven of the fifteen countries have introduced the second dose of vaccine and no reintroduction has taken place since 2015. Based on several parameters, the authors of this study estimate that 12 of the 15 countries do not meet the criteria for achieving the objective of eliminating measles. This is food for thought, as they also note that countries like Cape Verde, Gambia and Ghana have made substantial progress.
Measles: a re-emerging disease
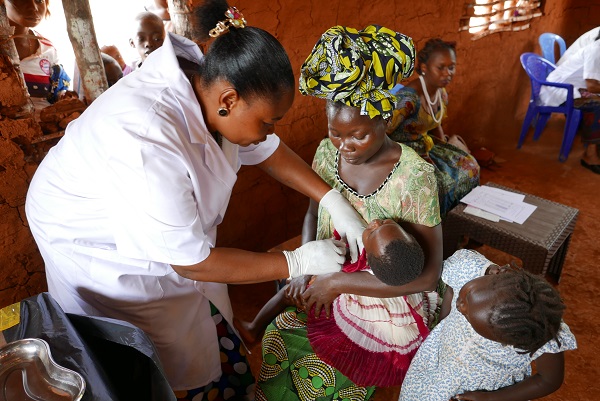
Measles is rife in several countries across the world. It mainly affects regions vulnerable to conflict and instability with substantial population displacement, where vaccination campaigns are disrupted. In addition, some forty countries postponed their measles vaccination campaigns for 2020 or 2021 due to the coronavirus pandemic (4). According to WHO, in 2020, more than 22 million infants did not receive their first dose of the measles vaccines, some three million more than in 2019 (3). Between April 2021 and April 2022, 21 major measles outbreaks were reported around the world. Since the start of 2022, numerous cases have been reported in Nigeria, India, Liberia, Ethiopia, Pakistan, Afghanistan, DRC, Somalia, Somaliland, Zimbabwe, Chad, Yemen and more.
MSF is involved in the response in Nigeria, Chad, Guinea, South Sudan, Somaliland, Afghanistan and Yemen.
Measles, MSF, Epicentre: a long history
War, instability and population displacement create the ideal conditions for outbreaks of this infectious disease. MSF has a long history of involvement in measles management and vaccination in many contexts. At the same time, Epicentre reports on epidemics occurring in these contexts, and evaluates vaccine coverage, mortality, the relationship with nutritional conditions and the use of the vaccine outside the cold chain.
Measles: an underestimated burden
Since 2008, Epicentre has been attempting to evaluate the actual burden of measles and identify those most vulnerable to the disease. Because although mortality from measles is low in developed economies, it remains almost certainly underestimated in other contexts. Death often occurs one month after infection and is frequently caused by pneumonia, so rarely attributed to measles.
An investigation (5) following a large measles outbreak in 2013 in the Aketi health zone in the Democratic Republic of Congo (DRC) showed:
- An attack rate of 14% (35% among children under five years) during the epidemic,
- A case fatality rate of 4.2% (6.1% among children under five years).
Furthermore, younger children, those who did not receive care, and those living farther away from Aketi Hospital early in the epidemic had a higher risk of measles related death. It should be noted that vaccine coverage prior to the outbreak was only 76% and a reactive vaccination campaign had taken place, but was delayed, which likely contributed to this high attack rate.
DRC’s national strategy for measles control relies on the Expanded Programme on Immunisation (EPI), including routine immunisation, regular supplementary immunisation activities (SIAs), and Outbreak Response Immunisation (ORI). But there are still many questions surrounding the implementation of these vaccination strategies, their timing, their geographical coverage, age groups to be considered, and the sequence of events.
Optimising vaccination strategies
The importance of vaccinating during epidemics
In 2008, an Epicentre study (6) showed the importance of vaccination during an epidemic in Niger, a previously debated subject. This study also showed that an increase in vaccine coverage and outbreak response vaccination results in longer intervals between major epidemics. In addition, an earlier response with lower coverage (~60%) appears more effective than a later response with higher coverage (>90%). Outbreak response vaccination is most effective where warning and monitoring systems allow the first signs of an epidemic to be detected as quickly as possible, which is rarely the case.
The complex question of detecting potential epidemics
For a response to be established, a warning threshold must first be determined and then exceeded in a specific geographical area. The difficulty lies in determining a warning threshold that is sensitive enough not to miss an epidemic, and specific enough to avoid false alerts.
Using the analysis of epidemics between 2018 and 2020 in DRC, Epicentre proposed a threshold with two options: either the detection of 20 suspected cases per week in a health zone, or 35 cases over three weeks. In the light of experience, and the existence of zones at high risk of epidemics, it seemed more appropriate to have more warnings, earlier, even if this bears a higher risk of false alarms.
This led to the inclusion of “high-risk zones” in the Urgepi project run in the regions of Haut-Lomami, Haut-Katanga, Tanganyika and Lualaba (formerly Katanga), which includes four types of activity:
- Surveillance of the whole area, but with a focus on high-risk health zones, in particular with earlier alert response and more detailed data collection.
- Alert response with measles kits, regular training for healthcare professionals in centres, and rapid intervention teams in case of a confirmed epidemic.
- Prevention with “catch-up” vaccination campaigns in high-risk areas.
- The opening of a laboratory in Lubumbashi to reduce diagnosis confirmation times. Laboratory-based confirmation of a measles diagnosis requires Elisa tests. However, until recently, one single laboratory in Kinshasa could carry these out, meaning several days or even weeks of transport for samples.

Initial experience showed that early detection with the sensitive threshold in high-risk areas enabled an intervention to be initiated before the epidemic progressed substantially, although not in all cases. It would therefore be interesting to see if including rapid diagnostic tests as an epidemic develops could facilitate more reliable, earlier detection and thus intervention.
Better vaccination targeting...
In countries at high risk of measles, supplementary immunisation activities (SIAs) are organised periodically to reach children who have not had a first dose or did not develop immunity following their first dose, which is the case for 20% of children. These SIAs often act as second doses for some children.
Prioritising vaccination means identifying zones where there are large numbers of non-immunised children, either because they have not been vaccinated or because they have not been exposed to the virus. A study carried out by Epicentre in DRC revealed that a combination of indicators such as vaccination coverage, time since last epidemic, and proximity to other potential epidemic outbreaks could guide this choice.
... thanks to seroprevalence surveys
Seroprevalence surveys can also be used to guide vaccination strategies. Quantifying antibodies, whether they are the result of exposure or vaccination, allows us to evaluate protection against measles in a given population. An Epicentre survey in four health zones in the former province of Katanga - now Haut-Lomami, Haut-Katanga, Tanganyika and Lualaba - after the 2015 epidemic showed a seroprevalence of 85% in children aged 5 to 14 years, with substantial area-dependent variations in children under five (7). These surveys revealed the low vaccination coverage of the Expanded Programme on Immunisation (EPI) in some areas, which could be the cause of the 2015 epidemic. The two zones with low seroprevalence in children under five experienced further epidemics in February 2016 and January 2017.
Serological surveys provide additional information that can be used to guide decision-making with regard to the need for and timing of SIAs. In February 2020, Epicentre re-evaluated immunity to measles in the Haut-Katanga region. Preliminary results, which must be confirmed, suggest a seroprevalence in children aged 6 months to 15 years of 59%, with no age-related difference. 81% had received one dose of the vaccine as part of the EPI or an SIA in 2019, increasing to 86% in under-fives. Despite SIAs, vaccination coverage remains too low and seroprevalence is lower than expected in children aged 5 to 15 years, despite their likely exposure to multiple epidemics.
These surveys show the importance of SIAs and response campaigns where vaccination coverage is low, and that the three-year interval between SIAs is almost certainly too long. The interval should be adapted on the basis of birth rate and vaccination coverage to reach the target of 95% vaccination, and thus specific to individual contexts.
In the same vein, a comparative analysis of the situation in Malawi and in DRC by MSF and Epicentre (8) shows the need to adapt the response to a measles epidemic to local epidemiology, stressing that the age distribution of early cases should guide the decision on which age groups to prioritise for vaccination. While non-targeted mass vaccination campaigns are usually the norm when it comes to epidemics, vaccination of young children, who are more likely to develop serious forms or die, should perhaps be prioritised.
A vaccine from the 1960s
The vaccine itself, and its storage, must also be considered. Measles epidemics most often occur in remote, sometimes insecure regions, making access difficult for vaccines that must be kept between 2 and 8 °C. Epicentre has shown that the vaccine can be kept for up to 6 days at 37°C or 2 days at 40°C in its single-dose lyophilised form (9). Whether this represents an operational advantage must still be established.
Others are looking into the development of a patch-based vaccine that would be easier to administer.
To sum up
Vaccination remains below the thresholds needed to eradicate measles in many countries, in particular DRC, one of the most affected by the disease. Limiting the risk of an epidemic requires improved EPI coverage, vaccination targeting, response times and SIA coverage as well as the establishment of context-appropriate alert thresholds.
Progress is being made in the fight against measles across Sub-Saharan Africa, but the re-emergence we have witnessed over recent years, which has accelerated since early 2022, just goes to show how precarious this progress is. Each country must establish its own priorities in terms of outbreak response and vaccination strategy based on local epidemiology. There is no one-size-fits-all solution, but rather a specific solution for each context.
Photo :Credit: Moses Sawasawa/Epicentre, Caroline Thirion/MSF, Juliette Muller/MSF
(1) Portnoy A Jit M Ferrari M Hanson M Brenzel L Verguet S. Estimates of case-fatality ratios of measles in low-income and middle-income countries: a systematic review and modelling analysis. Lancet Glob Health. 2019; 7: e472-e481
(2) Wariri O Nkereuwem E Erondy NA et al. A scorecard of progress towards measles elimination in 15 west African countries, 2001–19: a retrospective, multicountry analysis of national immunisation coverage and surveillance data. Lancet Glob Health. 2021; 9: e280-e290
(4) https://www.cdc.gov/globalhealth/measles/data/global-measles-outbreaks.html
(5) Gignoux E, Polonsky J, Ciglenecki I, Bichet M, Coldiron M, Thuambe Lwiyo E, Akonda I, Serafini M, Porten K. Risk factors for measles mortality and the importance of decentralized case management during an unusually large measles epidemic in eastern Democratic Republic of Congo in 2013. PLoS One. 2018 Mar 14;13(3):e0194276. doi: 10.1371/journal.pone.0194276. eCollection 2018.
(6) Ferrari MJ, Grais RF, Bharti N, Conlan AJ, Bjørnstad ON, Wolfson LJ, Guerin PJ, Djibo A, Grenfell BT. The dynamics of measles in sub-Saharan Africa. Nature. 2008 Feb 7;451(7179):679-84. doi: 10.1038/nature06509.
(7) Keating P, Carrion Martin AI. Blake A, Lechevalier P, Uzzeni F, Gignoux E, Okonta C, Langendorf C, Smit C, Ahuka C, Suchard M, Pukuta E, Degail ME, Hansen L, Kibanza-Kyungu J, Ciglenecki I, Cohuet S. Measles seroprevalence after reactive vaccination campaigns during the 2015 measles outbreak in four health zones of the former Katanga Province, Democratic Republic of Congo. BMC Public Health 2019 Aug 22;19(1):1153. doi: 10.1186/s12889-019-7500-z.
(8) Measles outbreak response immunization is context-specific: insight from the recent experience of Médecins Sans Frontières. Minetti A, Bopp C, Fermon F, François G, Grais RF, Grout L, Hurtado N, Luquero FJ, Porten K, Sury L, Terzian M.PLoS Med. 2013 Nov;10(11):e1001544. doi: 10.1371/journal.pmed.1001544. Epub 2013 Nov 5.PMID: 24223523
(9) Evaluation of the stability of measles vaccine out of the cold chain under extended controlled temperature conditions. Juan-Giner A, Alsalhani A, Panunzi I, Lambert V, Van Herp M, Gairola S. Vaccine. 2020 Mar 4;38(11):2473-2477. doi: 10.1016/j.vaccine.2020.02.005.






