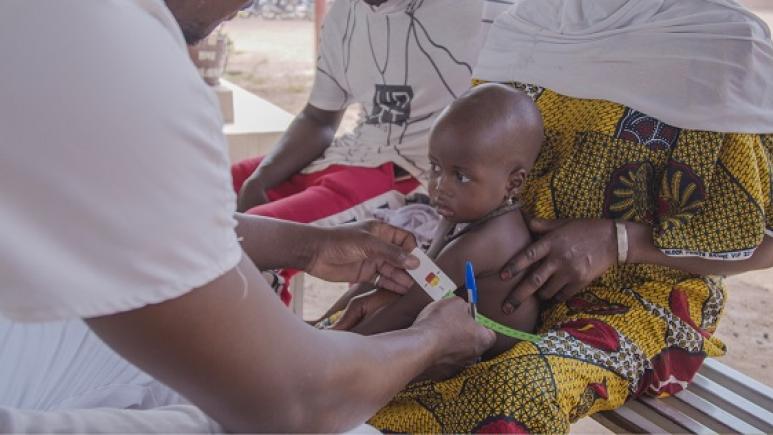
StimNut or how to adapt psychosocial stimulation for malnourished children in Mali
Acute malnutrition, alone or in combination with other diseases - malaria, diarrhea, respiratory tract diseases, so-called opportunistic infections - remains one of the leading causes of mortality among young children in Mali. In 2021, the prevalence of acute malnutrition was 10% in children under 5 years of age and the prevalence of severe acute malnutrition was 1.8%, according to data from the anthropometric nutritional survey and retrospective mortality survey conducted in December 2021 by Instat (1).
Beyond nutritional management
The management of malnourished children is based on medical treatment and nutritional care. But severe acute malnutrition (SAM), particularly in the first 1,000 days of life, has other serious consequences, including increased vulnerability to infection and diseases, increased early mortality, and motor and cognitive impairments, associated with behavioral and communication problems.
“These developmental delays are due to nutritional deficits, but also to a lack of emotional and psychosocial stimulation, says Dr. Jean-Gilbert NDONG, Medical Coordinator of Médecins Sans Frontières in Bamako. Early psychosocial stimulation of malnourished infants and young children has been shown to have short- and long-term benefits on cognitive and social development.”
For this purpose, Action contre la Faim (ACF) (in English Action Against Hunger) developed a five-session structured psychosocial stimulation intervention for children with SAM in the Follow-Up of Severe Acute Malnourished children (FUSAM) protocol. Between 2014 and 2017, this research project was implemented in Nepal to evaluate the effectiveness of a brief psychosocial intervention on child nutrition, health, and development: it showed the benefit of a combined nutritional and psychosocial intervention (StimNut) compared with an intervention based on nutritional treatment alone in children aged 6-23 months with uncomplicated SAM admitted to the community-based acute malnutrition management program in Saptari district (2,3). The psychosocial intervention included communication and play sessions; breastfeeding and feeding practices; massage, bathing, sleeping, and relaxation needs; and a family sharing session.
StimNut: psychosocial stimulation adapted to needs in Koutiala
 Psychosocial stimulation is part of the Integrated Management of Acute Malnutrition Protocol in Mali. However, it is rarely offered to children and their families due to a lack of expertise and resources, as well as a lack of appropriate protocols.
Psychosocial stimulation is part of the Integrated Management of Acute Malnutrition Protocol in Mali. However, it is rarely offered to children and their families due to a lack of expertise and resources, as well as a lack of appropriate protocols.
"With the support of MSF, the Malian Ministry of Health, and the NGO AMEDD (Association Malienne d'Éveil au Développement Durable, Malian Association of Awakening to Sustainable Development) , we will adapt FUSAM interventions to the Malian context and evaluate their feasibility and acceptability in Koutiala for children aged 6 to 23 months with severe acute malnutrition," explains Claire Bossard, Epicentre epidemiologist and study coordinator.
Médecins Sans Frontières has been working in this region of south-eastern Mali since 2009, where infant mortality was very high, providing medical and nutritional care to young children in the Koutiala hospital and in more than 30 community health centers in the region.
The first part of this three-part study consisted in describing the key factors, perceptions, norms and practices influencing the nutritional status and early development of young children. "Based on this assessment, we are now working on the second part of the study, namely the adaptation of the FUSAM protocol through a participatory research approach involving health workers, nutrition program managers, parents, traditional practitioners, key informants and the researchers involved in the study," explains Dr. Aissatou Diallo, study coordinator in Koutiala. The participatory approach will help us make this intervention both relevant and culturally appropriate, so that it meets the expectations of caregivers and stakeholders. By the end of 2022, the third part of the study - the implementation of the adapted psychosocial stimulation intervention - will be rolled out to 25 to 30 families. Weekly sessions between parents or caregivers of severely malnourished children and psychosocial agents, trained to accompany families, will be held in the two health centers selected for the study and the pediatric ward of the MSF hospital in Koutiala. The aim will be to sensitize parents or caregivers to the importance of stimulation, play, and a quality attachment relationship between the child and parent in the child's recovery process.
The acceptability and feasibility of integrating the adapted version of FUSAM will then be measured with the health personnel involved in its implementation and the parents or caregivers who have benefited from it.
This pilot study can then be extended to a larger number of children with SAM in the Koutiala district, and it should also provide a framework for adaptation to other settings.
Photo Credit: Mohammad Ghannam/MSF
- https://www.instat-mali.org/fr/publications/enquete-nationale-nutritionnelle-anthropometrique-et-de-mortalite-retrospective-mali-smart
- Le Roch K. Research Brief FUSAM: A Nutrition and Psychosocial trial for Treatment of Children with Uncomplicated Severe Acute Malnutrition in Nepal. 2018;(April 2019).
- ELRHA. Follow-up of severely malnourished children (FUSAM): effectiveness of a combined nutrition psychosocial intervention on health and development [Internet]. 2017 [cited 2021 Jul 22]. Available from: https://www.elrha.org/project/acf-fusam-nepal-call2/